Stress Incontinence In Women
JOIN OUR NEWSLETTER
Receive custom tools to help you manage your condition and get the latest in bladder and bowel health from NAFC!
Stress Urinary Incontinence In Women
Stress Urinary Incontinence is when pressure (or stress) placed on the bladder causes urinary leakage. This often happens with physical movement. If you’ve ever wondered why you pee when you laugh, pee when you cough, or pee when you exercise – that’s stress urinary incontinence.
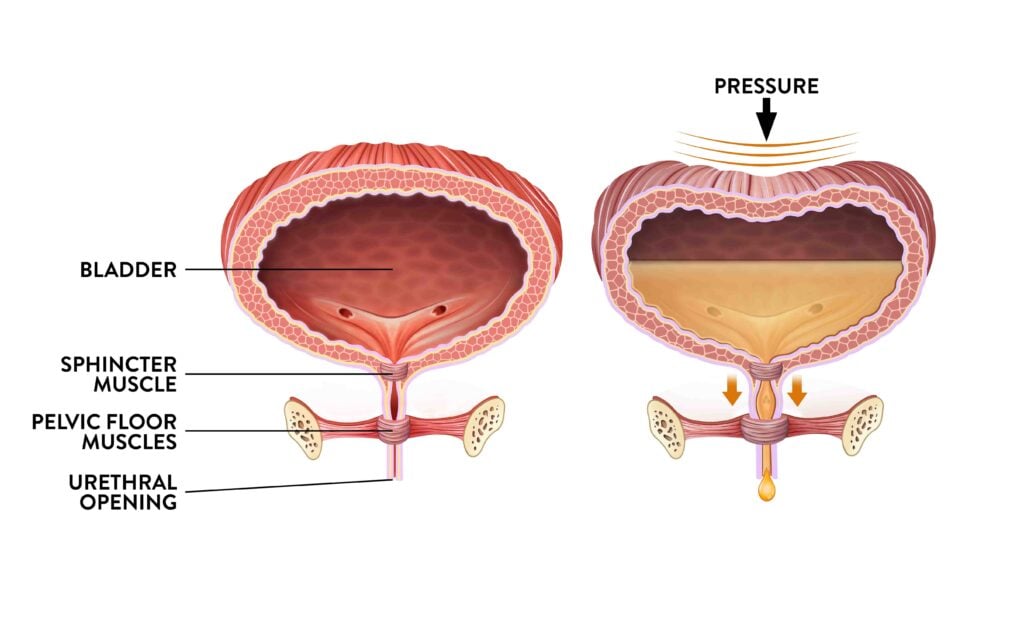
In order to understand why Stress Urinary Incontinence (also referred simply as “stress incontinence” or “SUI”) occurs, a quick refresher course on the female urinary anatomy might be helpful. The bladder has two functions. The first is to store urine produced by the kidneys and the second is to contract and push the urine through the urethra. Controlling the flow of urine out of the bladder is the sphincter muscle. The nervous system detects when the bladder is ready to be emptied and tells the sphincter to relax, allowing you to pee. When there is any sort of abdominal stress on the pelvic organs—the bladder, vagina, uterus, and rectum—SUI can occur.
It is important to understand the difference between stress incontinence (SUI) and urge incontinence (UUI) as they are treated differently. While Urge incontinence (UUI) involves the sudden and unstoppable loss of urine, SUI is not accompanied by the sensation of a sudden urge to urinate. The underlying cause for stress incontinence is different from that of UUI. Stress incontinence is caused by a weak sphincter muscle and/or pelvic floor. Some people have both SUI and UUI, known as mixed incontinence. This means that they leak urine when they cough, sneeze, or exert pressure on their abdominal muscles; but they also feel the urgent need to go to the toilet and may not make it in time.
Symptoms Of Stress Urinary Incontinence
Women with stress urinary 
Coughing
Sneezing
Laughing
Exercising or Working out
Having sex
Lifting something heavy
Standing up
Getting in or out of a car
Leakage may include just a small drop or two of urine or even a whole stream. Any amount is unwanted, so don’t dismiss your concerns simply because your leakage doesn’t seem as bad as it might otherwise be. If you find yourself wet, you can find yourself a treatment option.
Causes Of Stress Incontinence In Women
Stress incontinence is the most commonly occurring form of incontinence in women under the age of 60 and accounts for more than half the cases. As we’ve mentioned, anything that creates pressure on the pelvic floor muscles and your bladder may cause urine leakage.
While pregnancy and childbirth head the list for causes of stress incontinence, there are other health factors that may put you at risk, too. They include:
Loss of pelvic muscle tone. This can often occur with aging or childbirth, although people of all ages can develop SUI.
Hysterectomy (or any other surgery that affects your pelvic floor)
Nerve and muscle damage from childbirth or surgical trauma
Obesity
Menopause
Chronic coughing due to smoking and lung disease
Anatomical predisposition
Repeated heavy lifting or high-impact sports
How Does Stress Urinary Incontinence AFfect Your Life?
Stress urinary incontinence can have a huge effect on your quality of life. The physical and emotional demands created by stress incontinence can leave you feeling exhausted, embarrassed, and even depressed. Some of the common byproducts of SUI are:
Depression. Many people with SUI are deeply ashamed of their condition and live in constant fear of having an accident. This can lead to them avoiding things they once loved, like hanging out with friends or family, attending social events, or even working out. This restrictive nature of SUI can lead to isolation, loneliness, and depression in many if left untreated.
Skincare Issues. Constant moisture, especially urine, can cause your skin to be irritated and sore. It’s important to use proper protection for incontinence to avoid this from happening. Absorbent pads with wicking materials help keep moisture away from the body and avoid irritation, while moisture barrier creams can help protect skin from coming into contact with urine.
Stress urinary Incontinence Treatment Options
There are many treatment options as well as simple management techniques that can help you get your life back the way you want it.
With the increased attention on incontinence issues, incredible progress and innovation has been made in the arena of products for everyday use. Items ranging from absorbents to urethral inserts can be just the thing you need to get back your confidence and get on with your life. Click here to read about the various products for stress incontinence.
Behavioral Modifications & Noninvasive Options
Physicians generally pursue non-invasive therapeutic interventions before attempting to treat SUI with surgery. Ask your physician if one of these might improve your condition:
Loss of Excess Weight (see Diet & Exercise). Obesity is a risk factor in developing stress urinary incontinence due to the extra pressure placed on the pelvic floor and the bladder. Following a healthy diet and losing weight can help ease symptoms.
Smoking Cessation. You already know that smoking can cause or contribute to more diseases than we could ever list here, but you might not realize that it’s also a real factor in the development of SUI. All that coughing can put stress on your pelvic floor, and that can lead to muscle weakness and leakage. Just one more reason why quitting today can make a meaningful difference in your life.
Pelvic Floor Muscle Exercises. Kegel exercises help to strengthen the pelvic floor muscles so you’re able to better hold in urine. Kegels can be hard to master and should be incorporated with a range of core exercises. In addition, pelvic floor exercises are not for everyone and can actually do more harm than good for some people. It’s a good idea to see a physical therapist to get a proper evaluation and to learn how to do these exercises correctly.
(Note: Talk to your PT about products that may be able to help you strengthen your pelvic floor. New innovative products can assist in helping you strengthen your pelvic floor muscles.)
Biofeedback. Biofeedback is often done in conjunction with Kegels. A physical therapist may use a biofeedback instrument to measure your pelvic floor strength and monitor your improvement.
Bladder Retraining. This involves timing your trips to the toilet and slowly increasing the length of time between each visit. This can lessen the amount of fluid you have in your bladder and also help condition your bladder to hold urine for longer periods of time.
Pelvic Floor Stimulation or E-Stim. This therapy delivers a small amount of electrical stimulation to the nerves and muscles of the pelvic floor and bladder to help them tighten or contract, thereby strengthening them.
Injection Therapy. This technique uses a bulking agent that’s injected into the tissues around the urethra to help close the sphincter without interfering with urination, helping to reduce leaks.
Pessary. This is a ring-like device that your doctor will fit for you inside the vagina. The device helps to support the base of the bladder to prevent urine leaks. This is especially helpful for those who may have experienced a pelvic organ prolapse.
Medications For Stress Incontinence
Though millions of individuals suffer from SUI, there are no FDA-approved pharmaceutical medications to treat the condition. A couple of off-label medications that have shown to mitigate some symptoms of SUI are imipramine and pseudophedrine. Duloxetine is the only medication used to treat SUI, but it is not FDA-approved for this indication in the United States.
Topical Estrogen. Your doctor may prescribe local, low dosage estrogen administered vaginally to gently lubricate the tissues of the vagina. Many clinicians observe improvement in symptoms of SUI in many women. This should not be confused with Hormone Replacement Therapy (HRT), which has been not proven to relieve incontinence in postmenopausal women.
Urethral Bulking

Bulkamid. Bulkamid is a urethral bulking agent that is used to treat SUI. It is a smooth, water-based gel that remains in the body over time, similar to a facial filler, without causing reactions in the surrounding tissue. The Bulkamid procedure consists of 3-4 injections into the wall of the urethra. Adding additional volume to the wall of the urethra helps prevent urine from leaking out of the bladder during normal daily activities. Here are some key things to know about Bulkamid:
- Highly effective with a 92% success rate1
- Long-lasting
- Outpatient procedure1 with no hospital stay2 and short recovery time3
For more information on Bulkamid, visit Bulkamid.com.
Surgical Treatment Options For Stress Incontinence

Surgical slings are the most common procedure to address stress incontinence. A piece of plastic mesh tape is inserted into the pelvis to support the urethra. This is a minimally invasive procedure that involves the placement of a small piece of polypropylene mesh around the pubic bones underneath the urethra. Some important facts about surgical slings are:
- Outpatient procedure
- 80-90% success rate6
- Women who plan to get pregnant may want to wait until after their last pregnancy to have SUI surgery.
- Up to 2 days hospital stay6
- Up to 6 weeks of recovery time6
You can read about the types of surgeries for SUI and what to expect on this dedicated page here.
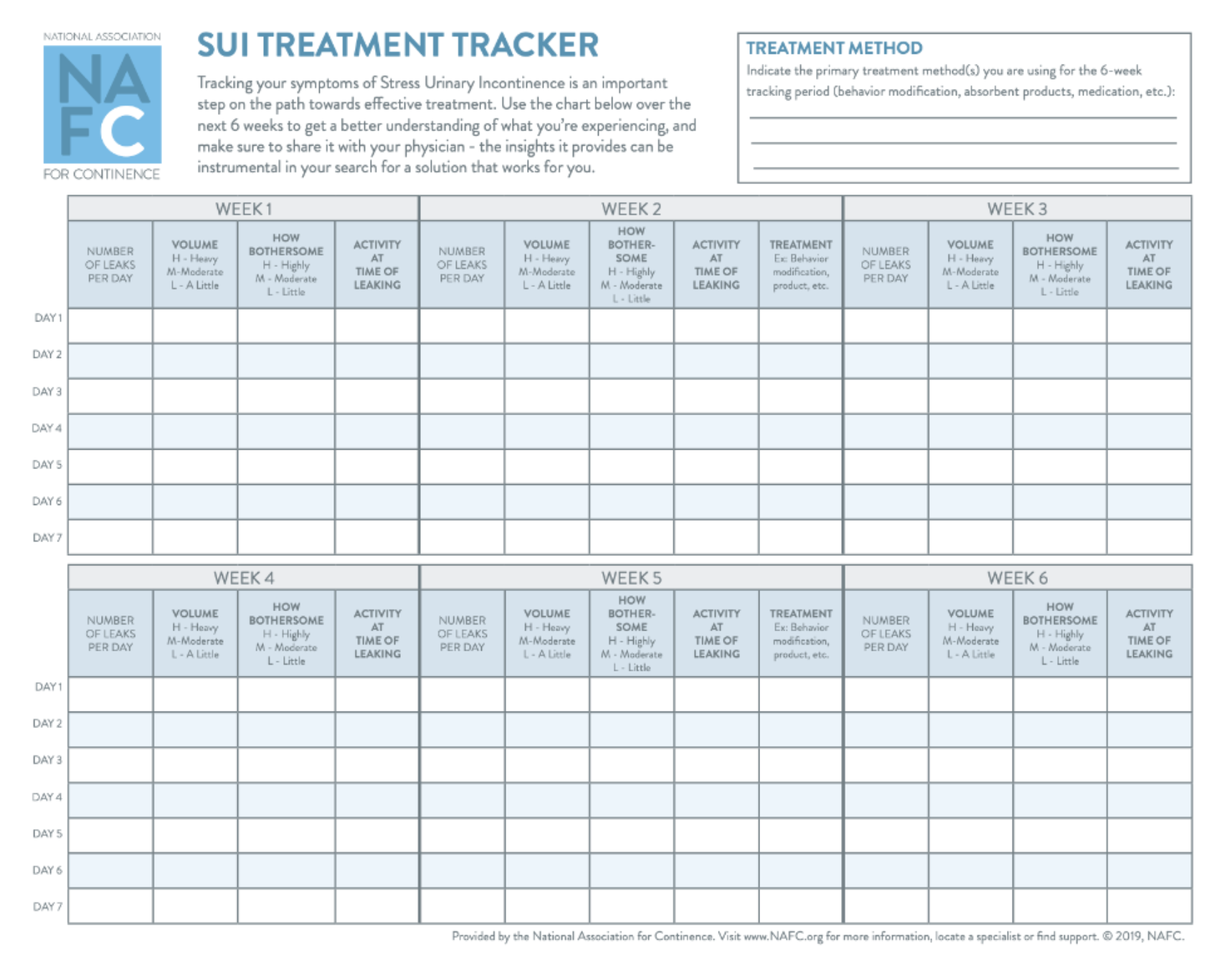
Track Your Progress
Whatever treatment option you choose, be sure to track your progress. NAFC makes this easy for you by offering a new SUI Treatment Tracker, which tracks your symptoms over a period of 6 weeks.
This tracker allows you to see your progress over the course of several weeks to see how you’re improving (or not) on your treatment plan. Once you’re done completing the sheet, take it to your doctor to evaluate your treatment options and to see if any changes may be needed. Sign up for this six-week program below, and receive free weekly reminders and tips from NAFC along the way!
Click Here To Get Your Treatment Tracker!
Talking TO Your Doctor About Stress Urinary Incontinence
You may feel hesitant to speak with your doctor about urinary incontinence, but you can rest assured that your doctor has likely treated many people with this condition – you’re not the first and you certainly won’t be the last to ask about SUI. Talking about your condition is the first step toward treatment, and it’s an important one, so it’s good to be prepared. Here are some things you can do to help make your visit more productive:
Track your symptoms. Click here to download an NAFC bladder diary and use it for at least 3 days, then take it in to your doctor. This will help inform your doctor of things like the severity of your bladder leaks and when you’re experiencing urine leaks, all of which may help to uncover any patterns happening with leakage.
Bring a list of any medications, vitamins or other supplements you are taking. Be prepared to talk about your doses and how often you take these medications.
Jot down a list of questions you want to ask. This can be a hard conversation to have and you may find yourself feeling anxious during your appointment. Having your questions at the ready can help ease your mind a bit and ensure that you don’t forget anything or leave important topics uncovered.
Do your research. Learn about all the various treatment options available to you and think about your preferences. Not ready for surgery? Make sure you tell that to your doctor. Interested in trying a new product? Let them know.
Demand treatment. There are a lot of myths out there about SUI, but one of the biggest is that it’s a normal part of aging. This couldn’t be further from the truth: SUI is common, but it’s NOT normal, and it’s NOT something you should have to live with.
Talk to a specialist. It’s very important to talk to a bladder specialist – most often a urogynecologist or urologist who knows how to diagnose and treat SUI. To find a specialist near you, visit www.FindRealRelief.com .
This page has been reviewed for medical accuracy by Lara S. MacLachlan, MD.
Sources
- The Lewin Group, Inc. National Women’s Health Resource Center 2007 2.
- Sokol ER, Karram MM, Dmochowski R. Efficacy and safety of polyacrylamide hydrogel for the treatment of female stress incontinence: a randomized, prospective, multicenter North American study. J Urol. 2014 Sep;192(3):843-9 3.
- Bulkamid Patient Information Leaflet 2021 OUS 110-0256-003rB 06/202
- Dwyer et al., “Voice your choice”: A study of women’s choice of surgery for primary stress urinary incontinence, International Urogynecology Journal (2020), 31:769-777. 2.
- Itkonen Freitas et al., Tension free vaginal tape vs polyacrylamide hydrogel injection for primary stress urinary incontinence: a randomized controlled trial., J Urol., 2020 Feb., Vol. 203, 372-378
- Mid-urethral Sling (MUS) Procedures for Stress Incontinence RV3. IUGA Patient Information Leaflet
RELATED ARTICLES

Ask The Expert: From A Doctor’s Perspective What Are Some Common Questions You Hear?
If you’ve ever sneezed and held your breath hoping for the best, you’re not alone. Bladder leaks, pelvic floor issues, and the constellation of symptoms that go with them are incredibly common — and incredibly under-discussed. We sat down with two of our favorite experts who are changing the bladder leak conversation: Dr. Barbara Frank, Attn: Grace medical advisor and board certified OB/GYN, and Dr. Sara Reardon, pelvic floor physical therapist (and the woman your pelvic floor has been waiting to meet). They took turns asking each other the questions their patients ask most — and answered them with the same candor they bring to the exam room. They cover everything from how to prepare for postpartum, to what question to ask your own pelvic floor PT, to how to manage incontinence during menopause. This is a knowledge drop you don’t want to miss.
Why So Many Women Put Themselves Last — and Why It Matters
Women are often the caregivers, planners, problem-solvers, and emotional anchors for everyone around them. They manage households, careers, children, aging parents, relationships, schedules, and responsibilities that rarely stop.
And somewhere in the middle of taking care of everyone else, many women quietly stop taking care of themselves.
They ignore symptoms. Delay appointments. Push through exhaustion. Normalize discomfort. Tell themselves they’ll deal with it “later.”
But later can turn into years.
This Women’s Health Month, it’s worth asking:
When was the last time you truly prioritized your own health

Is Bladder Leakage a Normal Part of Aging?
There is a quiet, widespread belief among women that at a certain age, after children, after menopause, and after “a lot of living,” bladder leaks just happen. You carry a pad. You know which restrooms are the cleanest. You skip the trampoline park with the grandkids. You don’t say anything to your doctor because, honestly, what would they even say? This is just…aging.
Using appropriate absorbent products and a gentle skin-care routine may help support skin integrity.
The medical community is clear: urinary incontinence is common, but it is not a normal or inevitable part of aging. The Mayo Clinic Health System states it directly that “although urine incontinence is common, it’s not normal.” The condition has causes, those causes have treatments, and those treatments, for many women, work remarkably well.

From Postpartum to Postmenopause: The Conversations Women Need to Have
In this episode of Life Without Leaks, we’re joined by Dr. Barbara Frank of Harvard Medical School and Brigham and Women’s Hospital, along with Alex Fennell, co-founder of Attn: Grace, an innovative manufacturer of incontinence products.
Together, we explore the realities of bladder leaks and pelvic floor health during pregnancy, postpartum recovery, perimenopause and menopause, and we discuss why more women are finally beginning to talk more openly about their experiences.
The conversation covers:
• The connection between hormones, menopause and bladder leaks
• Why pelvic floor therapy is having a major moment
• The surprising relationship between pelvic floor tension and incontinence
• How products can impact skin health, comfort and UTIs
• The truth about hormone replacement therapy
• Why community and conversation matter so much in women’s health
Alex also shares the story behind Attn: Grace and the company’s mission to create cleaner, plant-based incontinence products designed to support women with comfort, dignity and confidence.
Whether you’re navigating postpartum recovery, menopause symptoms or simply looking to better understand pelvic health, this episode offers expert insights, practical advice and an encouraging reminder that no one should feel alone in these experiences.