Millions of Americans experience some form of incontinence. And, while this condition affects both genders, if you are a woman, you are more likely to suffer from incontinence than men due to things like pregnancy, childbirth, and menopause.
There are several different types of incontinence you may experience:
-
Stress Urinary Incontinence: SUI occurs when any extra pressure placed on your bladder or abdomen causes you to leak urine. Things like sneezing, laughing, or certain exercise all may trigger SUI.
-
Urge Incontinence: Also known as Overactive Bladder, Urge Incontinence is the sudden, frequent feeling that you need to use the restroom.
-
Mixed Incontinence: Many people suffer from both Stress Urinary Incontinence and Urge Incontinence combined.
-
Urinary Retention: This type of incontinence occurs when you are unable to completely empty your bladder, leading to leaks.
The good news is that all of these conditions are treatable. And now, more than ever, there are countless options for treatment, so if you haven’t yet found something that works for you, try again! Here are some popular treatment options:
-
Absorbent products: Probably one of the most widely used treatment options, absorbent products are a good first line treatment for those who experience leaks. There are many different types and fit is very important, so expect to try out a few and see what works best for you. And whatever you do, don’t use sanitary pads in place of absorbent products specifically designed for leaks – the two are made of different materials and sanitary pads are not designed to hold urine, so leaks are likely to occur if you use them for that purpose.
-
Behavioral Therapy: Before trying out medication or other procedures, you may want to tweak some of your behaviors to see if they have any effect. Things like altering your diet to eliminate bladder-irritating foods, starting a physical therapy routine, or practicing bladder retraining can all have an effect on managing your symptoms.
-
Medications: There are a number of medications that may help you with bladder control. Most medications work by calming the bladder and reducing the spasms that sometimes happen and cause leakage. Talk with your doctor about the different types and learn what may work best for you.
-
Non-invasive procedures: If you’ve tried medications and have not seen results, or experienced unwanted side effects, you may want to give a non-invasive procedure a try. InterStim, Botox, and PTNS are all simple procedures that can be administered in a urologist’s office and can have a significant effect on symptoms and quality of life. Talk with your doctor to learn more about these procedures and what you can expect if you choose to go this route.
-
Surgery: Several surgical options exist for those experiencing urinary incontinence. Surgery is often a more permanent solution, and is a common approach for many who have failed on other treatment plans. But, it’s not for everyone, and may not always eliminate all your symptoms. Be sure to talk to your doctor (usually a urological surgeon) about what may work for you and what you can expect after surgery.
Finding the best treatment plan for you requires you to play an active role. Know your options and educate yourself about the different treatments available so you are better able to discuss them with your physician and make an informed decision together.
To find a specialist in your area, visit the NAFC Specialist Locator and make an appointment today!
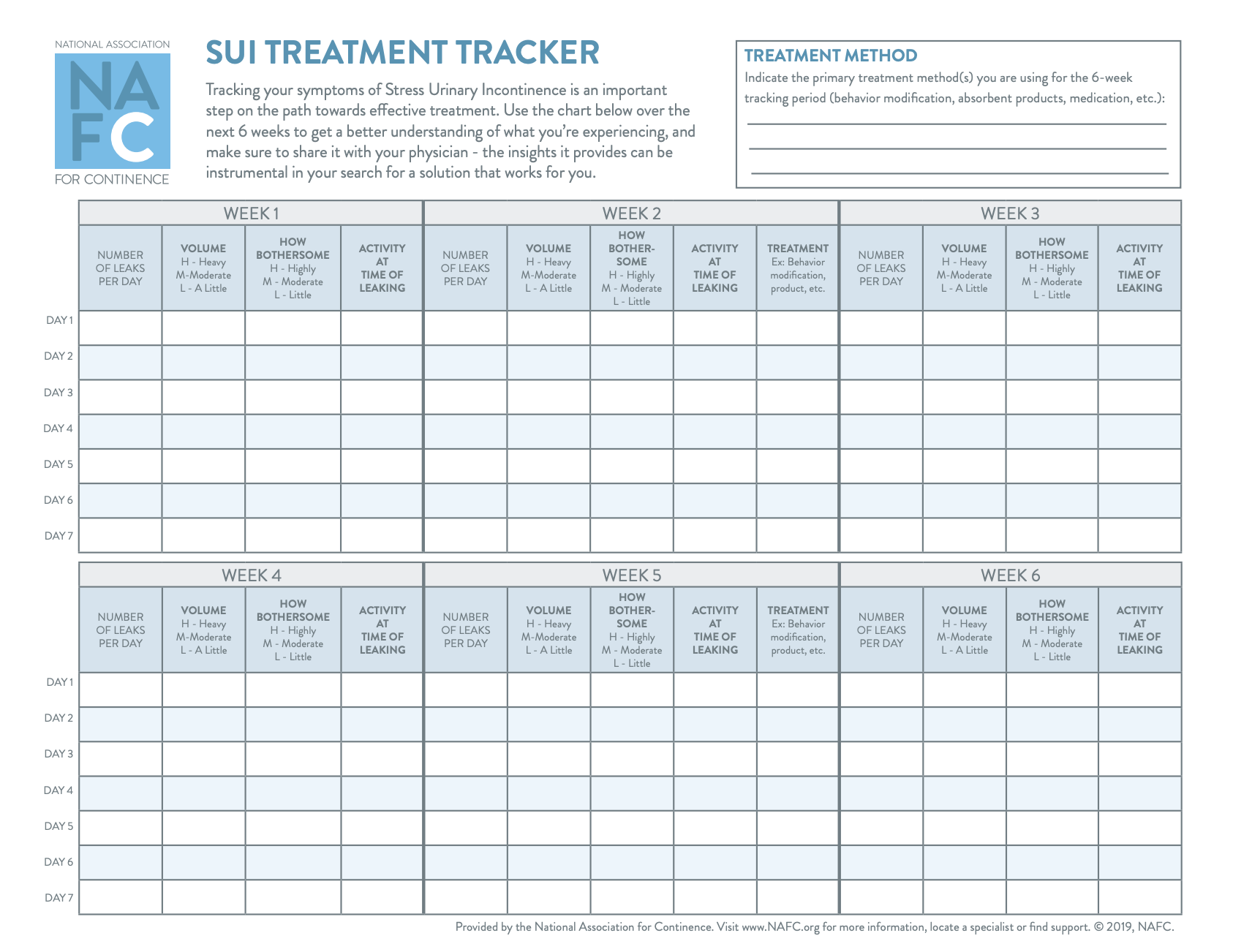
SUI TReatment Tracker
SIGN UP TO RECEIVE THE SUI TREATMENT TRACKER!
Have you started treatment for SUI? Sign up to receive our SUI Treatment Tracker and keep track of your progress! This 6 week program will help keep you on track and will help determine how your treatment is working.
Sign Up To Download The SUI Treatment Tracker Here!









One Response
Great article on something that a lot of people with this problem don’t want to talk about. There are so many products on the market, how do you know which is best for you. Wearever – http://www.weareverincontinence.com – provides a full range of products and lots of advice and information to help you make informed decisions.